PSORIATIC ARTHRITIS
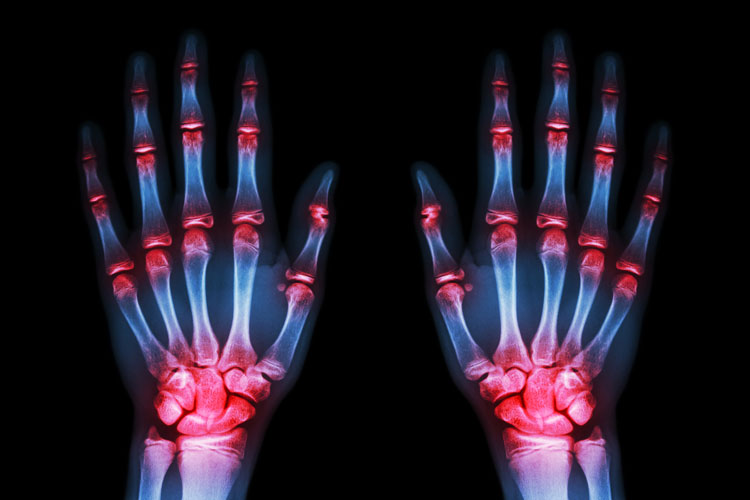
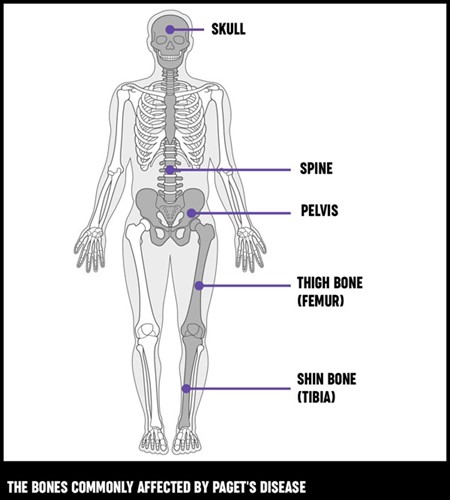
Psoriatic arthritis is an autoimmune disease in which your immune system attacks your joints and skin, causing pain, stiffness and swelling. It most commonly affects the fingers, toes, wrists, knees, ankles and lower back.
It occurs equally in males and females. About 30 percent of people who have psoriasis, another autoimmune disease that causes itchy, scaly rashes on the skin. In fact, the skin disease precedes the arthritis in nearly 80% of people. However, the arthritis may precede the psoriasis in up to 15% of patients.
For more information on Psoriatic Arthritis, visit the Arthritis Foundation at www.arthritis.org.

Symptoms of Psoriatic Arthritis:
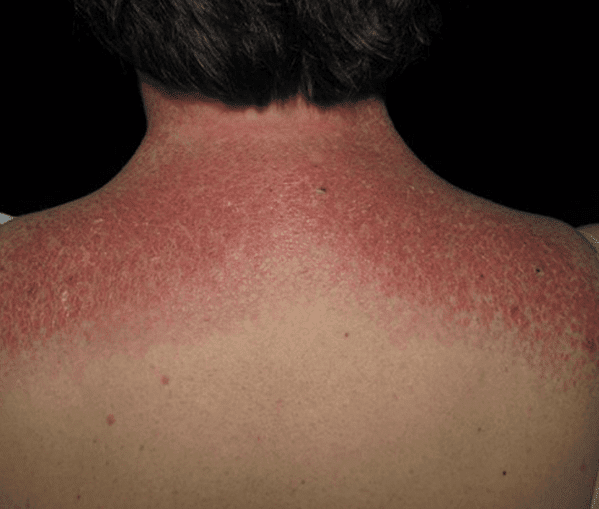
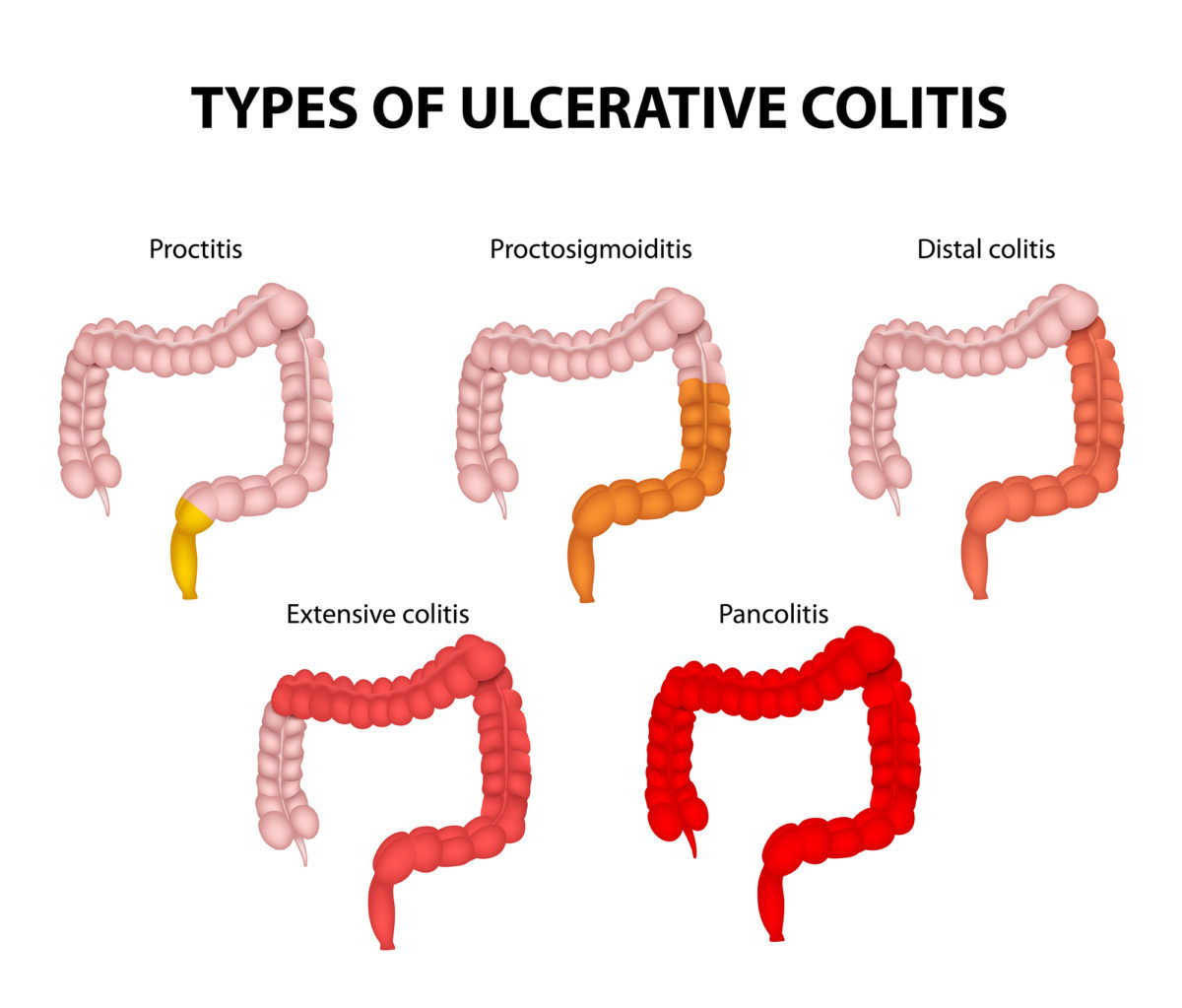
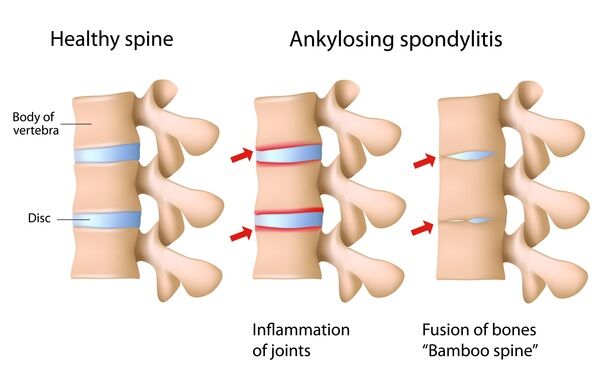
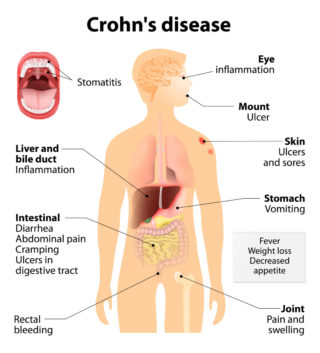
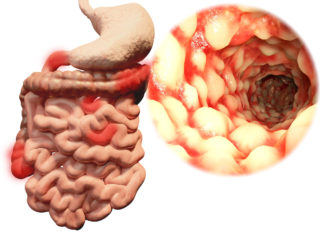
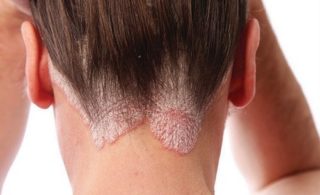
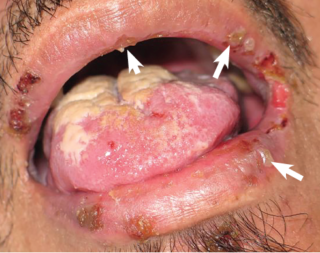
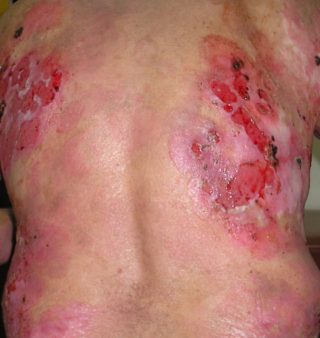
Psoriatic arthritis shares many symptoms with several other arthritic conditions, such as ankylosing spondylitis, reactive arthritis, and arthritis associated with Crohn’s disease and ulcerative colitis. Psoriatic arthritis presents as red patches of skin topped with silvery scales and additional symptoms include:
- Low back pain
- Conjunctivitis
- Reduced range of motion
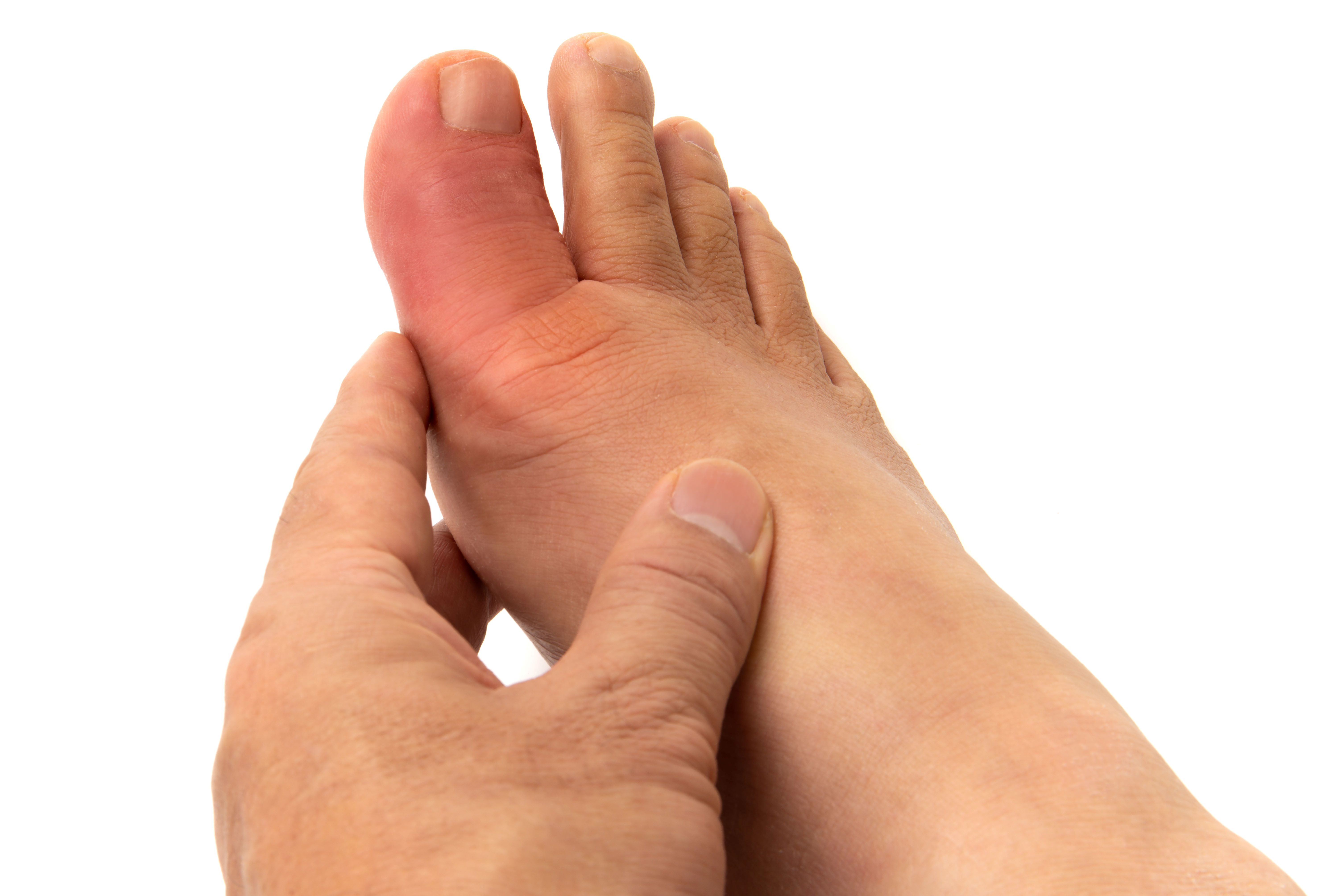
- Swollen joints
- Nail pitting
- Joint pain and morning stiffness
- Foot pain
- Fatigue
Diagnosis of Psoriatic Arthritis:
Psoriatic arthritis is a diagnosis made mainly on clinical evaluation and based on the finding of psoriasis along with the typical inflammatory arthritis of the spine and/or other joints. There is no laboratory test to diagnose psoriatic arthritis. Some blood tests may confirm an abnormal elevated result and merely reflect presence of inflammation in the joints and other organs of the body. When one or two large joints (such a knees) are inflamed, arthrocentesis can be performed. This is an office procedure whereby a sterile needle is used to withdraw fluid from the inflamed joints. The fluid is then analyzed for inflammation. X-rays may show changes of cartilage or bone injury indicative of arthritis of the spine, sacroiliac joints, and/or joints of the hands. The blood test for the genetic marker HLA-B27, is often performed. This marker can be found in over 50% of patients with psoriatic arthritis who have spine inflammation.